Recently, the Inflation Reduction Act (IRA) is getting a lot of attention, particularly for its provision that allows CMS to start drug price negotiation for selected drugs 9 (small molecules) or 13 (biologics) years after drug launch. However, the Centers for Medicare and Medicaid Innovation (CMMI) has proposed a number of a number of payment models intending to address pharmaceutical cost, spending, and reimbursement. In fact, in 2023 CMS proposed 3 new models to reduce out-of-pocket (OOP) cost for Medicare and Medicaid beneficiaries. These previous initiatives are nicely summarized in a paper by Liu et al. (2024).
Most recently, in response to President Biden’s February 2023 executive order, CMMI proposed 3 new models related to drug prices: (i) Medicare High-Value Drug List, (ii) Cell and Gene Therapy (CGT)Access model, and (iii) Accelerating Clinical Evidence model.
- Medicare High-Value Drug List. Medicare Part D sponsors would provide access to 150 high-value generics drugs that treat chronic conditions by assuring by providing a standard set of ~150 drugs for no more than $2 each per month. These generics would not be subject to utilization management. Note that it is voluntary for Part D plans to participate in this program.
- CGT Access Model. This model allow CMS (at a federal level) to bargain with drug manufacturers on behalf of a of state Medicaid agencies (SMA) and also negotiate & administer “outcomes-based agreements.” Each SMA can decide if they want to participate in each agreement. This approach is currently being implemented for sickle cell disease gene therapies.
- Accelerating Clinical Evidence Model. When FDA grants drugs accelerated approval based on clinical trials data using surrogate endpoints, CMS would pay lower reimbursement rates for these drugs until confirmatory trials were completed.
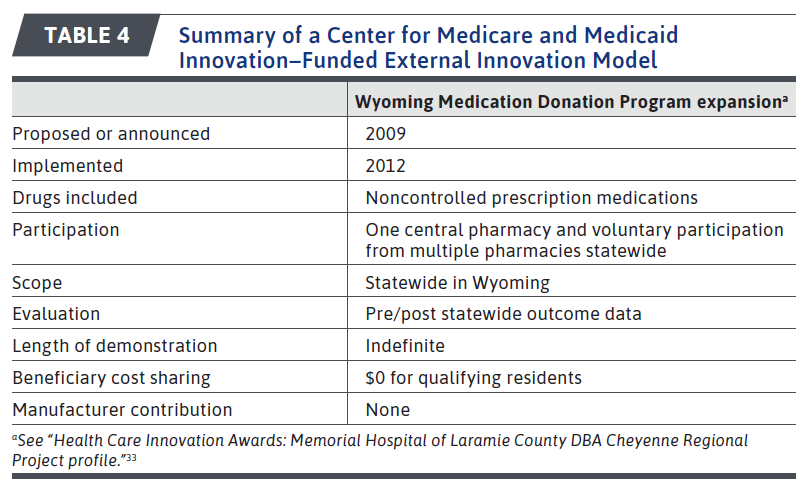
Prior to the development of these models, CMMI also proposed 9 other drug pricing models. Three of these models related to Medicare Part B drugs and 5 related to Part D drugs. The last program was an externally funded program in Wyoming. Summaries of each of these are in the tables below. None of the Part B proposals were implemented (0/3), but four of the Part D proposals (4/5) were have been implemented.
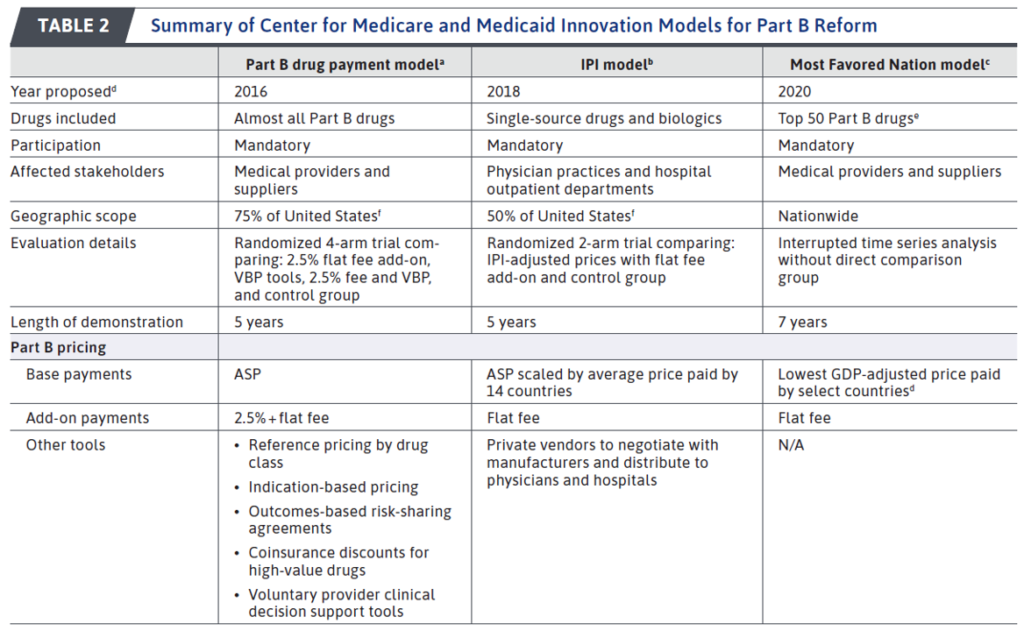
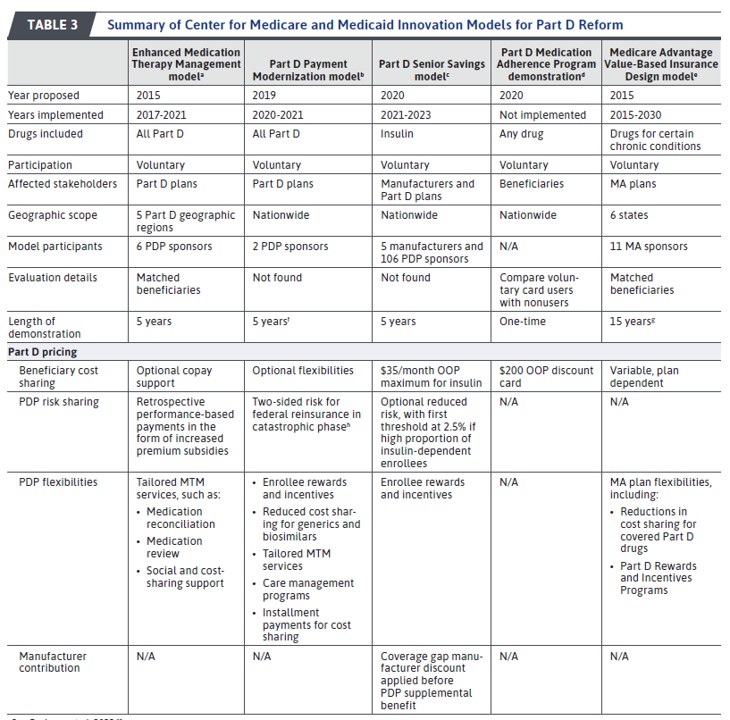
The impact of the implemented programs was mixed. [Note that because no Part B model was implemented, there was no impact from those proposals.]
- The Enhanced Medication Therapy Management model included 6 prescription drug plans (PDPs) and aimed to incentivize increased use of MTM services (e.g., medication reviews, refill reminders, and physician education) in order improve adherence and reduce adverse events. However, the model “…produced no clear effect on total medical expenditures or medication adherence.”
- The Part D Payment modernization model aimed incentivize Part D plans to reduce cost in the Part D catastrophic phase. The model imposed 2-sided risk in the catastrophic phase, with PDPs eligible to share in 30%-50% of savings below a target benchmark but being responsible for 10% of excess costs. “The model was designed as a 5-year demonstration, but it was terminated after 2 years because only 2 health plans participated nationwide, presumably because of concerns of excess costs or logistical complexity.”
- The Part D Senior Savings Model lowered cost sharing for to $35 per month and allowed Part D plans to share brand name discounts in the coverage phase with beneficiaries. While this program greatly reduced beneficiary OOP cost, it has been supplanted by IRA, which also imposes a $35/month maximum cost sharing for insulin and also revised the Part D benefit schedule.
- The Medicare Part D Medication Adherence Program Demonstration was not implemented. It proposed that Part D beneficiaries would get a one-time $200 drug discount card.
- Medicare Advantage Value-Based Insurance Design (VBID) model is the only on-going model. It allowed Medicare Advantage plans to restructure their benefit designs around VBID principles (lower cost-sharing for high-value drugs and services). Of the 11 participating MA plans, 3 used VBID for Part D drugs through the “Part D Rewards and Incentives Programs”. Did the program work? The Liu et al. paper found that “beneficiaries in programs with interventions showed a 1.6% increase in 30-day medication fill rates and decreases in the probability of hospitalization (8.8%) or emergency department admission (5%). However, this association was not observed for the same outcomes when matched comparators were compared with individuals in non-VBID plans, casting some doubt on whether the CMMI intervention was the cause of the differences observed.
The one externally funded program was a 3-year grant to the Wyoming Institute of Population Health. The program aimed to transform rural health care delivery through the creation of medical neighborhoods. The program included mail order pharmacy services at no additional cost for low-income, uninsured or underinsured Wyoming residents.
In short, while IRA is getting the headlines today, the Liu et al. (2024) paper highlights that CMMI been attempting to impact pharmaceutical spending and beneficiary OOP cost for many years. To date, the success of these programs is mixed at best.






